NCDC says late treatment and weak health-seeking behaviour are pushing
deaths higher across 23 states, with five states accounting for 84% of cases.
The Nigeria Centre for Disease Control and Prevention (NCDC) issued an updated Lassa fever
situation report this morning that put the year’s death toll at 191, with health officials sounding a
fresh alarm over what they say is now one of the worst Lassa seasons on record.
According to the report, which covers Epidemiological Week 18 (April 27 to May 3), the case
fatality rate has climbed to 24.6 percent — up sharply from 19.2 percent during the same period
in 2025. In plain terms: roughly one in four people who test positive for Lassa fever in Nigeria
this year is dying.
The geography of the outbreak tells its own story. Confirmed cases have now been recorded in
23 states across 106 local government areas, but five states — Bauchi, Ondo, Taraba, Edo, and
Benue — account for 84 percent of all infections. These are the historic hotspots, and the
NCDC says they are once again straining under the weight of detection, isolation, and treatment
demands.
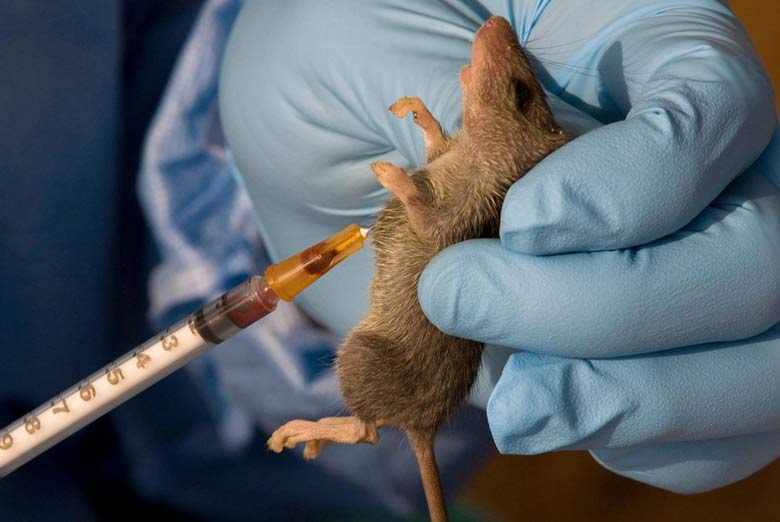
Lassa fever is endemic to West Africa, but Nigeria carries the heaviest burden. The virus is
carried by the multimammate rat (Mastomys natalensis), which sheds the pathogen through
urine and droppings into food stores, water, and household surfaces. Most years see a sharp
dry-season spike between January and April; what is unusual about 2026 is that the curve is
failing to come down on schedule.
In its statement, NCDC pointed to two drivers behind the rising fatality rate. The first is late
presentation: many patients arrive at treatment centres only after days of fever, body aches, and
bleeding — by which time the antiviral ribavirin, the standard of care, has dramatically reduced
efficacy. The second is what officials call “poor health-seeking behaviour,” with families selfmedicating, consulting traditional healers, or attributing symptoms to malaria until the disease is
advanced.
There is also a quieter problem the situation report acknowledges: capacity. Nigeria has only a
handful of treatment centres capable of managing severe Lassa cases, and several of them are
in the same five hotspot states already overstretched. The Irrua Specialist Teaching Hospital in
Edo — long the country’s reference site for Lassa — has been operating at high occupancy for
weeks. Health workers themselves are at elevated risk, and the NCDC has flagged nosocomial
transmission as a concern in at least three states.
The economic and human costs are climbing alongside the case count. Lassa survivors
frequently report long-term complications, including partial or permanent hearing loss in up to a
third of cases, and households often shoulder treatment costs out of pocket. In rural areas, lost
wages during isolation can push families below the poverty line within weeks.
NCDC Director-General Dr Jide Idris has urged Nigerians to seek care at the first sign of
unexplained fever, especially in the hotspot states, and to avoid bush meat consumption and
improper food storage. The agency has reactivated its Emergency Operations Centre and is
coordinating with state ministries of health on intensified rodent control campaigns and houseto-house risk communication.
Politically, the outbreak is creating an uncomfortable backdrop for the Tinubu administration’s
health sector reforms. The government has been touting renewed investment in primary
healthcare, but the Lassa numbers are a reminder that surveillance, laboratory capacity, and
rural clinic readiness remain uneven. Opposition voices, including PDP figures who have been
vocal in the lead-up to 2027, are already framing the toll as evidence of a broader public health
drift.
There is, however, a small piece of good news buried in the data. The pace of new infections in
some hotspot states has slowed week-on-week, suggesting that intensified community
engagement is beginning to land. The question is whether that deceleration can outrun the case
fatality rate, which historically lags new cases by two to three weeks.
For now, public health experts say the immediate priority is straightforward: get patients into
treatment faster. Every extra day before ribavirin is administered shifts the survival math against
the patient. Until Nigeria closes that delay, the death toll will likely keep climbing.